Even though there are many genital psoriasis treatment options available, treating genital psoriasis may be difficult due to the sensitivity of the skin affected by this autoimmune disease.
Page Contents
Is Genital Psoriasis Contagious?
Genital psoriasis is not an STD and it is not contagious. The most common type of psoriasis that people experience in the genital area is inverse psoriasis. followed by plaque psoriasis
In both men and women, in addition to the classic appearance on the elbows, knees, hands, feet, and the lower back, the symptoms can also manifest themselves in almost all other parts of the body, for example on the scalp or in the genital area.
Up to 63% experience psoriatic lesions in their genital area at least once during their lifetime.
Genital psoriasis differs from classic psoriasis (psoriasis Vulgaris) in part in terms of its symptoms, treatment, and possible consequences.
Many patients do not report the symptoms out of shame and doctors do not ask questions out of uncertainty or ignorance. The topic often remains undiscussed, which increases the suffering even more.
Below are some pictures of genital psoriasis:
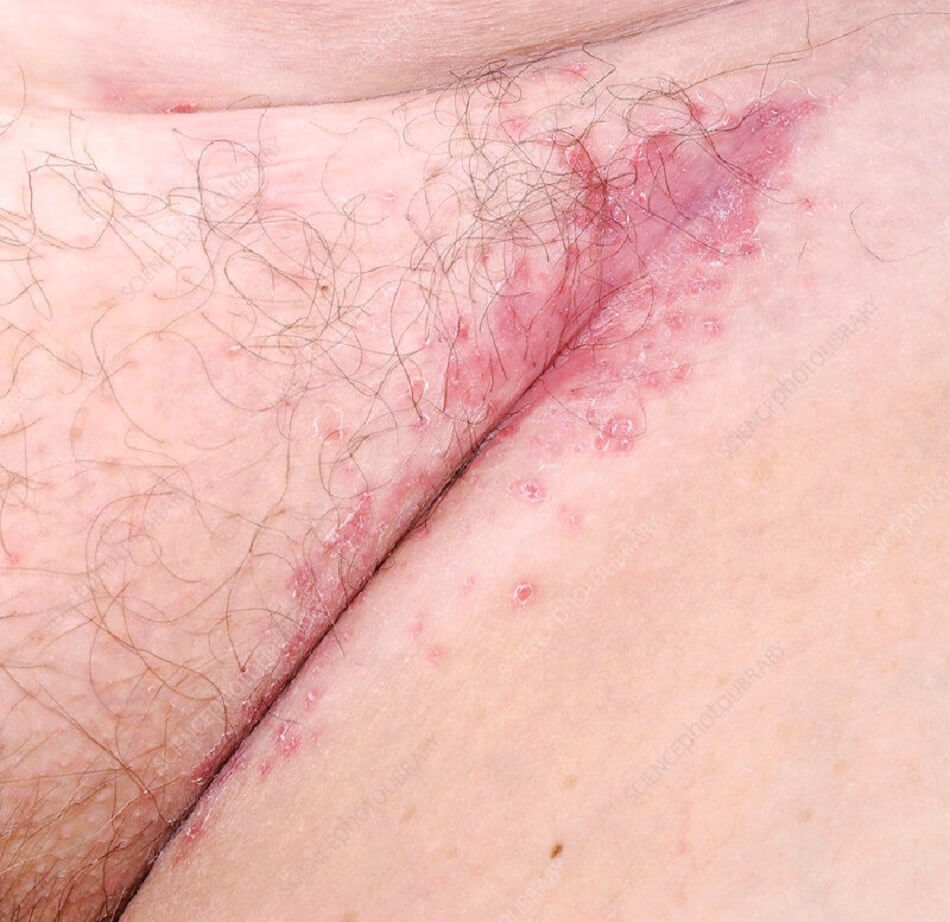
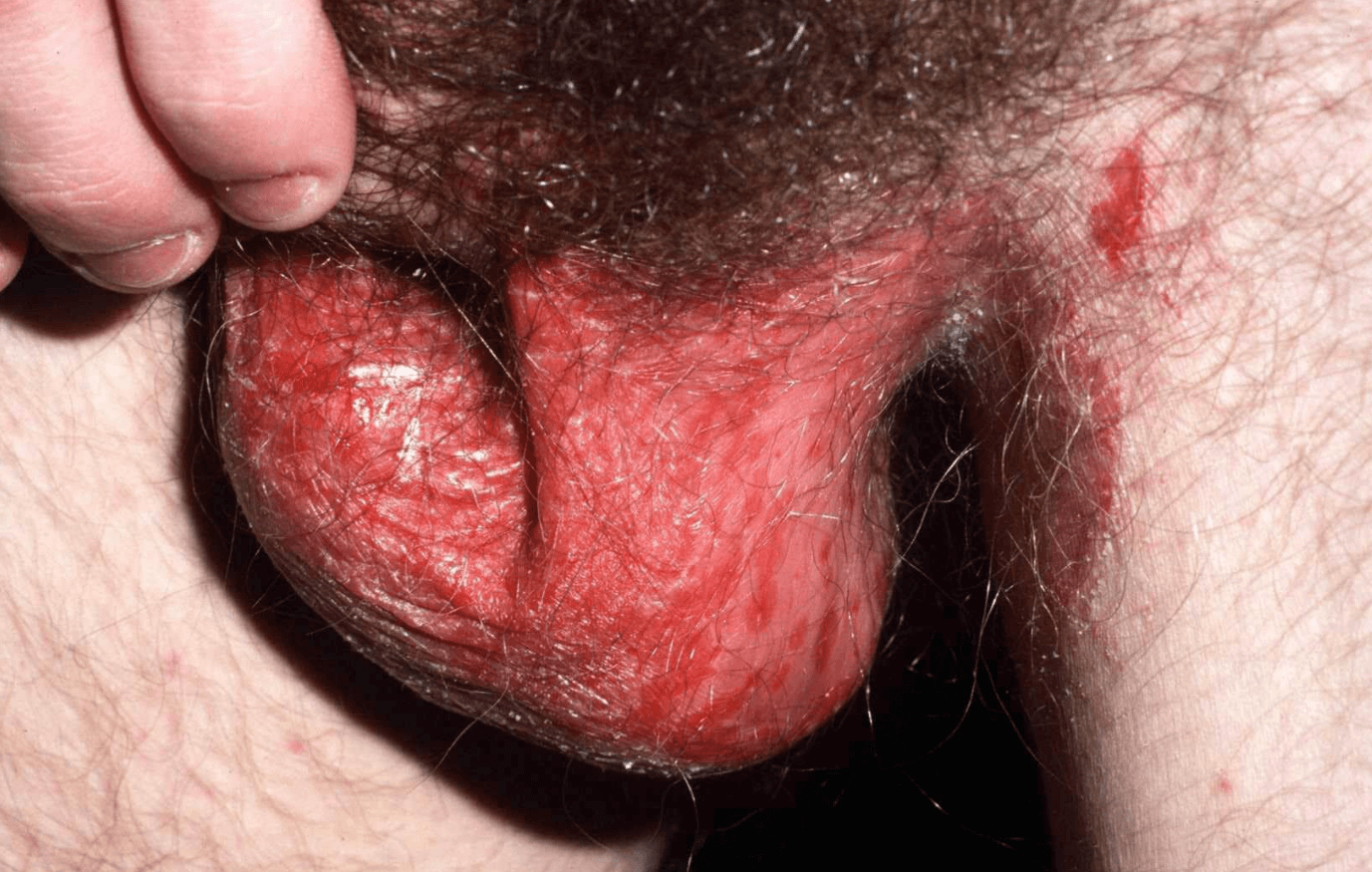
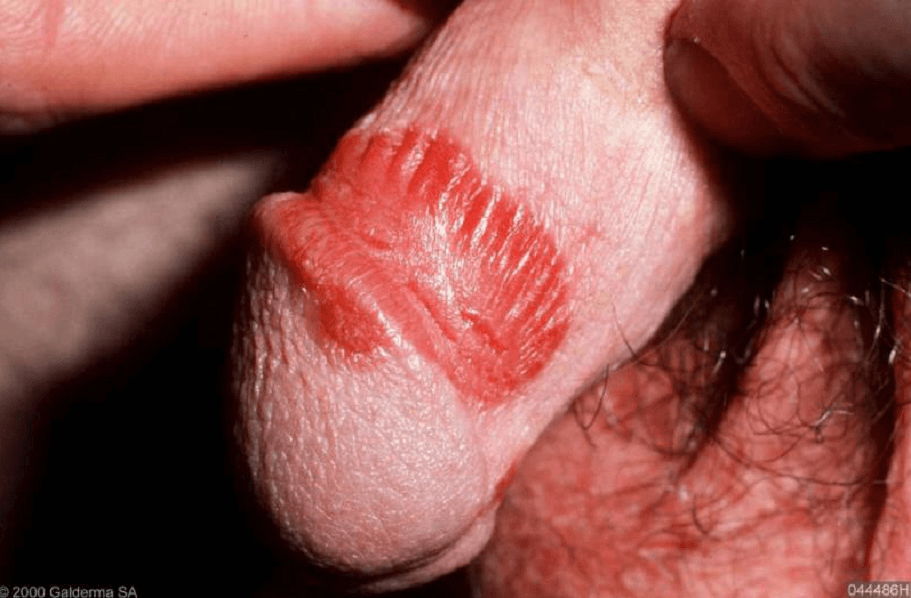
Genital Psoriasis Symptoms
The main symptom of genital psoriasis is reddened, often very itchy, sometimes burning and sometimes painful skin changes in the area of the genitals and anus.
The dry flaking typical of psoriasis does not usually occur in these areas.
When psoriasis occurs in the genital and anal areas, it is usually weeping rather than dry there. Often it is particularly difficult to treat and also associated with high levels of suffering.
Genital psoriasis can be very itchy which is very disturbing. It can keep you up at night. You could even scratch the itchy areas in your sleep until you bleed. This can cause a cycle of more itching and bleeding, which in turn increase the risk of an accumulated infection with bacteria and/or fungi.
Genital psoriasis can also be accompanied by burning and stinging. Sweat, heat, and friction make this feeling worse. The more you move or sweat, the more irritated your skin becomes. Any participation in sports can worsen the symptoms. For some people, even sitting can hurt.
It is not uncommon for bacterial colonization of the plaques. In addition, the risk of fungal infections is increased.
Genital Psoriasis in Women
When psoriasis spreads to the genital area in women, the vulva is affected and vulvar psoriasis often appears smooth, non-scaly, and red.
While it can cause itching, it is important not to scratch the area as it can cause infections and dry skin. This infection can lead to thickening of the skin and additional itching.
Genital psoriasis usually does not affect the mucous membranes and often remains on the outer layer of the vaginal skin.
Genital Psoriasis in Men
In men, genital psoriasis usually affects the penis. Especially the penis root and/or the testicles show typical skin changes in the case of an illness.
Men can get small red spots on the shaft or tip of their penis. Scaly patches are more common when you’ve been circumcised.
The affected skin areas are very sensitive and can become sore and bleed when touched or rubbed.
Genital psoriasis also affects other areas.
Psoriasis in the anal and surrounding areas
The first sign of psoriasis in the anal opening or anal fold is itching, which those people who are affected, find unbearable.
In addition, the skin between the buttocks is often torn and can bleed.
Patients with psoriasis in the area of the anal folds have an increased risk of accompanying psoriatic arthritis, which often manifests itself as painful, swollen joints, morning stiffness in the joints, and/or painful tendon attachments.
The folds of the buttocks may show heavy scaling and redness. The skin is less sensitive but still difficult to treat.
The area between the thigh and groin
Psoriasis appears in this area as non-scaly, red, and white in the folds between the thigh and groin.
The skin may also crack. Those who are overweight or those who practice athletics can also get an infection in the folds of the skin that resembles a fungal infection.
Psoriasis on the thighs manifests as small, round patches that are red and scaly. Irritation can occur with psoriasis in this area, especially in people whose thighs rub together when they walk or run.
Diagnosing Genital Psoriasis
The appearance of genital psoriasis differs from psoriasis in other parts of the body.
Usually. your doctor or dermatologist can make a diagnosis just by looking at the skin.
Not so, however, with genial psoriasis. It can resemble various fungal infections or, in some cases, inflammatory skin and connective tissue diseases.
To confirm genital psoriasis, your doctor may perform a skin biopsy and have it examined in a laboratory.
Psychosocial Consequences
Genital psoriasis is very uncomfortable and stressful for both sexes affected by it.
Studies have shown that the suffering of psoriasis patients with symptoms in the genital area is much higher than that of patients with no genital symptoms.
Because of the pain and shame, many sufferers often avoid all sexual contact. This can have further negative psychosocial consequences such as conflicts in a partnership or even loneliness.
To prevent this from happening, patients are urgently advised to have an open conversation with their partners. Inhibitions towards the life partner are out of place here and can only further limit the quality of life.
Sexuality is – with restrictions due to the symptoms – also possible with genital psoriasis, especially if this is treated well.
You should therefore under no circumstances feel ashamed to tell your doctor.
The doctor can only prescribe the appropriate treatment when he knows about all of your complaints and knows about psoriasis in the anal or genital area.
Not every therapy that is commonly used for psoriasis is also suitable for treating genital psoriasis. You should therefore avoid hasty self-treatment as far as possible.
Genital Psoriasis Treatment
Although treating genital psoriasis is difficult, there are many genital psoriasis treatment options available.
The skin in the pubic area is very thin and delicate. This must be taken into account when deciding on the treatment.
In particular, products that you have been prescribed primarily for the treatment of other parts of the body should not be used in the genital area without consulting your doctor.

1. Topical treatments
Ointments and/or creams are applied to the psoriasis patches, such as:
- Corticosteroids (hormone ointment)
Sensitive skin areas, which include the vagina, penis and glans, and the anal area, should normally not be treated with highly effective cortisone.
Why? In the genital region, for example on the penis, the skin is extremely thin. This has the following consequences:
- Active ingredients like cortisone are absorbed much easier by thin skin
- The cortisone then makes the skin even thinner
- Makes the skin is more prone to side effects
If your doctor decides cortisone treatment for your genital psoriasis makes sense, the doctor will normally prescribe weak or medium-strength creams containing cortisone. These are:
- Mild strength corticosteroids (Desonate gel, Desowen cream)
- Medium strength corticosteroids (Westcort cream, Dermatop cream, Pandel cream)
Due to the high rate of fungal colonization, a combined cortisone/anti-fungal agent is often used in the treatment.
However, the application should be slowly “tapered off” after a maximum of two weeks. This means that the intervals between the individual applications are getting longer and longer. Using this ointment for too long can cause stretch marks and broken vessels.
If the cortisone treatment is stopped abruptly, psoriasis can flare up, and usually more severe.
Sometimes anti-inflammatory, cortisone-free preparations from neurodermatitis treatment are also used, as these can be used for a longer period without fear of the skin becoming thinner.
Ointments and/or creams are applied to the psoriasis patches, such as:
- Vitamin D3 creams (Calcitriol)
A vitamin D cream has fewer long-lasting side effects than a hormone ointment, and you can use it for a longer period of time. Sometimes they are mixed with a mild corticosteroid ointment to make it less irritating. Not all vitamin D creams are good for sensitive skin, so only use the cream your doctor prescribes.
- Calcineurin inhibitors
Calcineurin inhibitors are agents that inhibit the increased activity of the immune system, which suppresses the inflammatory reactions of the skin and reduces rash and itching.
Calcineurin inhibitors are normally used for moderate to severe atopic eczema, but they can also work for genital psoriasis.
These medicines. eg. Elidel (1% strong pimecrolimus) and Tacrolimus 0.1% ointment do not contain hormones, so they are safe to use on your penis and vagina. Expect a stinging and burning sensation when you first apply them to the skin.
- Mild coal tar
Sometimes prescribed when the topical steroid prescribed proves to be inefficient.
NOTE: Always use topical treatment as prescribed by your doctor to avoid side effects.
2. Systemic Therapy
Systemic drugs are powerful drugs that can affect your entire body. not just the skin. Your doctor may also prescribe them if the psoriasis is very severe or not well controlled, or if you also have severe psoriasis on other parts of your body.
Systemic therapy is very rarely the initial treatment used for genital psoriasis, but like psoriasis on the rest of the body, psoriasis in the pubic area can respond well to it.
Treatments are taken as tablets or administered by injection or infusion.
Systemic treatments include, for example, methotrexate and cyclosporine.
3. Biologics
Biologics are relatively newer drugs that specifically target the way your immune system works. They are artificially produced proteins from the body.
Treatments are administered by injection or infusion. An example is Ixekizumab (Taltz)
These treatments include, for example, methotrexate, cyclosporine, fumarates, and biologics.
Unsuitable treatments for genital psoriasis
Some treatments used to treat body psoriasis, are not suitable for genital psoriasis. These include Anthralin and light therapy.
Here are some tips on how you can support genital psoriasis treatment:
In addition to drug treatment, it is important to avoid additional skin irritation at all costs.
In no case should you give in to the itching and scratch the affected areas. If germs or pollutants penetrate into scratched areas of the skin, the inflammation worsens.
- Wear loose, comfortable clothing that does not fit or chafe too tightly at the crotch.
- When exercising, give preference to breathable underwear in which sweat does not accumulate.
- Do not shave your intimate area, as this unnecessarily irritates the genital area.
- If possible, avoid long periods of sitting or walking and change your position often.
- Avoid rough, damp, and/or scented toilet paper.
- Regularly clean the anal and genital area carefully and thoroughly with lukewarm water and avoid using irritating care products.
- If necessary, take hip baths with artificial tanning agents. They have anti-inflammatory effects and relieve itching.
Conclusion
Talk about genital psoriasis.
Complaints of the skin in the pubic area are not always easily discussed.
Patients often walk around with the complaints for a long time without consulting their doctor. This often happens out of shame. Nevertheless, it is important to tell your doctor if you have complaints in the pubic area.
Your doctor is not surprised and can diagnose and treat the condition appropriately.

Emotional aspects
Genital psoriasis can have a major impact on quality of life. Psoriasis in this intimate area can cause a lot of psychological distress in addition to physical complaints.
Itching from genital psoriasis can be present throughout the day and is extremely bothersome for many patients. Living with itching in the genital region is not an easy task. There is a tendency to want to scratch, which is not always possible in public. This often makes patients feel desperate. In addition, people can be insecure due to skin disease or the treatment. They may feel very embarrassed.
Research among many psoriasis patients shows that genital psoriasis can also have a major impact on the (sexual) relationship.
It is not easy for everyone to speak about these topics.
Nevertheless, you can also contact your doctor about this. Depending on your problems, and if needed, your doctor can refer you to a medical psychologist or sexologist. These care providers can help you accept and learn to deal with your skin disease and its consequences for your (sexual) quality of life.